- “Chronic Kidney Disease Basics.” Centers for Disease Control and Prevention, Centers for Disease Control and Prevention, 28 Feb. 2022, www.cdc.gov/kidneydisease/basics.html.
- Kazancioğlu, Rumeyza. “Risk Factors for Chronic Kidney Disease: An Update.” Kidney International Supplements, U.S. National Library of Medicine, Dec. 2013, www.ncbi.nlm.nih.gov/pmc/articles/PMC4089662/.
- MM;, Salem. “Pathophysiology of Hypertension in Renal Failure.” Seminars in Nephrology, U.S. National Library of Medicine, pubmed.ncbi.nlm.nih.gov/11785065/
- “Health Problems Caused by Kidney Disease.” American Kidney Fund, 10 Nov. 2023, www.kidneyfund.org/living-kidney-disease/health-problems-caused-kidney-disease.
- “Mineral and Bone Disorder.” National Kidney Foundation, 11 Feb. 2021, www.kidney.org/atoz/content/MineralBoneDisorder.
Risk Factors & Complications of Chronic Kidney Disease
February 23, 2026
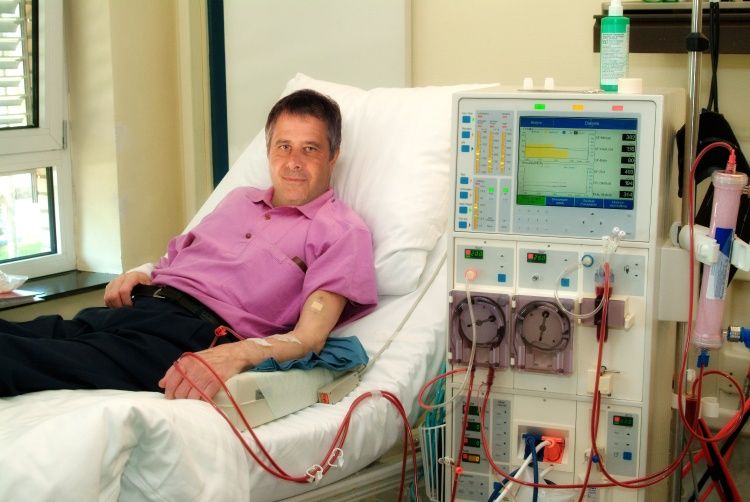
At a glance:
Genetics, Ethnicity, Age, and Gender:
Inherited genes, ethnic background (especially African descent), natural age-related kidney decline, and male gender can increase risk for CKD and ESRD.
Lifestyle Factors:
Smoking, heavy alcohol use, obesity, high blood pressure, diabetes, and overuse of pain relievers all raise the likelihood of developing CKD.
Complications:
CKD can lead to high blood pressure, anemia, weakened bones, heart disease, and fluid buildup, impacting overall health.
Prevention and Management:
Early detection, regular checkups, and lifestyle modifications can slow CKD progression and protect kidney and heart health.
Chronic Kidney Disease (CKD) is a significant health concern affecting more than one in seven American adults, roughly 37 million people. These vital organs play a crucial role in filtering the entire blood supply every half hour. When kidneys are damaged, as is the case with CKD, they struggle to efficiently remove waste and excess fluid. This can lead to potential health complications such as heart disease and an increased occurrence of infections. ¹
This condition varies in seriousness but tends to worsen over time. CKD can result in anemia, increased infection risks, and disruptions in blood chemicals, impacting overall well-being. Fortunately, early detection, lifestyle changes, and appropriate medical interventions can slow its progression. This introduction will shed light on CKD, emphasizing the importance of understanding risks and potential complications associated with this prevalent health issue. ¹
Risk Factors
Factors such as genetics, race, age, family history, and lifestyle choices contribute to CKD risk. Smoking, obesity, hypertension, diabetes, and exposure to certain substances increase vulnerability. Read on for the need for early detection and intervention to address modifiable risk factors and prevent CKD progression. ²
Genetics & Ethnicity
Some people inherit genetic changes that affect how well their kidneys function. For example, mutations in the Uromodulin gene can impact a protein that is normally found in urine. Variations in the APOL1 gene, which are most commonly seen in people of African descent, are linked to a significantly higher risk of developing end-stage renal disease (ESRD), especially from certain types of kidney damage. Other genes involved in blood pressure regulation, including those in the renin–angiotensin system such as angiotensinogen, may also increase risk in certain populations.
Ethnicity also plays an important role. African Americans have a higher risk of developing ESRD compared to Caucasians, particularly when high blood pressure is the underlying cause.
Recognizing how genetics and ethnicity affect kidney health allows healthcare providers to develop more personalized care plans and identify individuals who may benefit from earlier monitoring or targeted treatment. ²
Family History & Socioeconomics
Your family history and socio-economic status can play a role in your risk of kidney disease. If you have close relatives with end-stage renal disease (ESRD), you might be at a higher risk, as nearly 23% of incident dialysis patients had family members with ESRD. Screening high-risk family members is advised to prevent kidney disease.
Socioeconomic factors like income, occupation, and education also matter. For instance, having an income below $16,000 compared to over $35,000 is associated with a 2.4-fold increase in CKD risk. Those from families with unskilled workers or with lower education levels also face higher CKD risks. Unemployment, especially among non-Hispanic blacks and Mexican Americans, is linked to a higher prevalence of CKD. Recognizing the influence of family history and socio-economic factors is essential for proactive kidney health management.²
Gender & Age
Gender and age significantly influence kidney disease risk, with studies indicating higher prevalence of end-stage renal disease (ESRD) among men. In a 10-year follow-up study in Okinawa, Japan, the odds ratio for ESRD was 1.41 for men compared to women, meaning men had a 41% higher likelihood of developing ESRD.
As individuals age, their renal function tends to decrease, making the elderly population more susceptible to chronic kidney disease (CKD) after various factors or events that can harm the kidneys. ²
Diabetes, Obesity & Hypertension
Obesity has been strongly linked to chronic kidney disease (CKD). Large studies show that people who are overweight at age 20 have about three times the risk of developing CKD later in life. Long-term obesity is associated with a three- to fourfold increase in risk. Extra weight places stress on the body by increasing inflammation, causing oxidative stress, and damaging blood vessels, all of which can affect the kidneys. Staying physically active and maintaining a healthy weight can help lower this risk.
Diabetes, a condition marked by high blood sugar levels, is the leading cause of CKD and end-stage renal disease (ESRD) worldwide. Many people who require hemodialysis have diabetes, which highlights how strongly the two conditions are connected. Keeping blood sugar levels under control is one of the most important steps in protecting kidney health.
Hypertension, or high blood pressure, is another major risk factor. Over time, uncontrolled high blood pressure can scar the kidneys and reduce their ability to function properly. When hypertension goes untreated for 10 years or more, it can lead to noticeable kidney damage. Managing blood pressure through medication, diet, exercise, and regular checkups is essential for preserving kidney function.
Understanding these risk factors makes it easier to take preventive steps and protect long-term kidney health.²
Smoking, Alcohol & Pain Killers
Smoking, alcohol use, and certain medications can all increase the risk of chronic kidney disease (CKD) leading to kidney failure over time.
Smoking harms the kidneys in several ways. It increases inflammation, reduces healthy blood flow, and damages the tiny filtering units inside the kidneys. Research shows that smoking more than 20 cigarettes per day significantly raises the risk of developing CKD. Even smaller increases matter. For every additional five cigarettes smoked per day, levels of serum creatinine, a marker of kidney function, rise by about 31 percent.
Heavy alcohol use can result in kidney damage. Recreational drug use, exposure to heavy metals, and overuse of pain relievers are additional risk factors. Analgesics are medications used to relieve pain, including common over-the-counter options. When taken excessively or for long periods without medical supervision, these drugs can significantly increase the risk of end-stage renal disease (ESRD).
Being aware of these lifestyle risks and using substances in moderation can help protect kidney function over time.²
Complications
Discovering and understanding the health problems associated with kidney disease is essential for comprehensive kidney health. Your kidneys play a crucial role in the overall functioning of your body, and when they face challenges, it increases the likelihood of other health issues. Common complications arising from kidney disease include hypertension, anemia, bone disease, heart disease, and fluid buildup.³
Hypertension
Kidney disease often leads to high blood pressure, also called hypertension. Traditionally, this was thought to happen because damaged kidneys struggle to remove salt and water. This causes extra fluid to build up in the body, which increases blood flow and triggers the blood vessels to tighten, raising overall blood pressure.
Recent research shows that the connection between kidney function, blood vessel resistance, and body fluid levels is more complex than we once thought. Knowing how kidney disease affects blood pressure is important for preventing and managing hypertension and protecting long-term kidney health. ⁴
Anemia
Anemia is a common concern for people with CKD. When your kidneys are damaged, they cannot make enough erythropoietin which causes red blood cells to drop. While anyone can develop anemia, it becomes more prevalent in the later stages of CKD, particularly in stages 3-5. Anemia tends to worsen as CKD progresses, and if your kidneys are not functioning optimally, the likelihood of developing anemia increases. If you suspect you may have CKD, it's crucial to discuss it with your doctor and undergo appropriate testing such as a blood test or urine test. Managing anemia and addressing its symptoms can significantly improve your overall well-being.³
Bone Disease
Healthy kidneys are essential for keeping bones strong because they help regulate important minerals in the blood. When the kidneys aren’t working properly, this balance can be disrupted, leading to a condition called mineral and bone disorder.
Imbalances in calcium and phosphorus can affect not just the bones, but also the heart and blood vessels. When kidney function declines, phosphorus levels in the blood rise and the body produces less active vitamin D. This causes the parathyroid glands to release too much parathyroid hormone (PTH). High PTH pulls calcium from the bones, making them weaker and more likely to break. Some of this calcium can also build up in the heart and blood vessels, increasing the risk of heart problems.
Understanding how kidney disease affects bones and minerals is key to managing these complications and protecting overall health. ⁵
Heart Disease
Kidney disease and heart disease often go hand in hand, creating a complex relationship. Kidney disease can contribute to heart disease because the heart has to work harder to pump blood to the kidneys. This increased workload on the heart can lead to various heart and blood vessel problems, affecting the overall pumping efficiency. Importantly, this connection is bidirectional, as heart disease can also cause kidney disease. It emphasizes the interdependence of kidney and heart health. For those on dialysis, heart disease stands as the most common cause of mortality. Recognizing and managing these connections is crucial for preventing and addressing heart-related complications in individuals with kidney disease. ⁴
Fluid Build Up
Kidney disease can lead to fluid build-up and various health complications. One such issue is gout, a form of arthritis causing joint swelling and pain, primarily in the toes. Gout results from elevated uric acid levels in the blood, a condition exacerbated by impaired kidney function in filtering the blood. High levels of phosphorus and potassium, vital minerals for bone health and bodily functions, can also occur with kidney disease. The kidneys usually balance these electrolytes to regulate fluid levels, but in kidney disease, imbalances can lead to harmful effects. Additionally, metabolic acidosis, characterized by an excess of acid in the body, is common in individuals with kidney disease due to reduced blood filtration. Understanding these connections is crucial for managing fluid-related complications and promoting overall kidney health. ⁴
A Proactive Approach
CKD presents a significant health concern affecting millions of Americans, with factors like genetics, ethnicity, family history, socio-economic status, and lifestyle choices influencing its risk. The kidneys, crucial for blood filtration, may face challenges leading to complications such as heart disease and fluid build up when damaged. Understanding modifiable factors like smoking, obesity, hypertension, and diabetes is crucial for prevention. Genetic influences, socio-economic factors, and gender-related risks underscore the need for personalized care strategies.
A proactive approach involves regular health check-ups, monitoring risk factors, and making lifestyle modifications. Early detection, lifestyle changes, and appropriate medical interventions can significantly slow CKD progression. By focusing on screening and early intervention, individuals can take charge of their kidney health and overall well-being.
Get in Touch
Learn more about how RenalX at Woodbine supports personalized care for patients in Alexandria, VA. Contact us today to schedule a tour or speak with a member of our care team.
The information provided in the article is for general informational purposes only. This information is not a substitute for medical advice. Accordingly, before taking any actions based upon such information, you are encouraged to consult with the appropriate professionals.




